The AnaConDa (short for Anesthesia Conserving Device) is a novel concept that essentially works on the same basic principle as an Artificial Nose or HME. It allows a cost-effective alternative to using an Anesthetic Machine in the ICU.
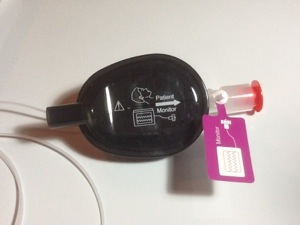
In my experience Anesthetic Machines are rarely used in the ICU. They have however been used for patients suffering from status asthmaticus and not responding to other treatments. To my knowledge Anesthetic Machines are usually brought into the ICU and used due to the bronchodilator effects (as well as the sedative effects) of the Volatile Anaesthetic Gases. The downsides to doing this have included the following:
1. It is a hassle to bring an machine to the ICU.
2. Often ICU staff are not as comfortable with an Anesthetic Machine as it is outside their “Normal” equipment.
3. Typically Anesthetic machines have limited modes of ventilation to deal with complex respiratory cases.
4. Often there is not be an uncommitted Anesthetic Machine available for the whim of the ICU staff.
The AnaConDa is a novel approach to providing an alternative to these issues with Anesthetic Machines.
How the AnaConDa works:
The AnaConDa functions like an HME with a charcoal bed as the medium to capture both expired moisture and Volatile Anesthetic Gases.
The AnaConDa is placed at the patient wye on the patient’s side (just like an HME). A syringe pump is loaded with a syringe containing a volatile anesthetic agent (sevoflurane or isoflurane) and then connected by a proprietary supply line to the inferior side of the AnaConDa where a small diffuser allows the volatile anesthetic agent to be introduced on the patient side of the AnaConDa filter. When the patient inspires the gas from the ventilator they also receive the Volatile Anesthetic Agent, when they expire both moisture and the Volatile Anesthetic Agent are trapped in the AnaConDa filter until their next inspiratory phase when they re-inspire the gas mixture with the previously expired moisture and Anesthetic Gas. It is a beautifully simple system. Some of the Volatile Gas will escape which means a scavenging system of some sort is required along with a slow and continuous infusion of Anesthetic Gas (via syringe pump) to replace what has been lost.

Other issues that need to be addressed.
1) You must be able to analyze the gas mixture to control the concentration being delivered to the patient (precise dosage is titrated for effect). Essentially you need a gas analyzer capable of analyzing the anesthetic agent you are using.
2) Not all the gas is captured by the AnaConDa requiring a scavenging system be used (either Active and Passive scavenging systems may be used).
Advantages to using an Volatile Anesthetic Agent for sedation.
Now this is where things get more interesting and also complex. Some of the advantages are very self-evident and probably subject to little controversy. Others are in various states of investigation and will vary in evidence (isn’t that always the case though?).
1. The primary reason I expect people to want to use this device will be for the bronchodilator effects it can provide on a continuous basis for patients with status Asthmaticus.
2. There are more reasons to use this device though than just Status Asthmaticus. Volatile agents are awesome sedatives. They have very fast onset and are easily controlled. You can put your patient to sleep or wake them up almost at will (15 to 20 minutes is what I am told for waking your patient). Drugs like Diprivan, Propofol and such can have along half life making it difficult to get your patient to wake up enough for a proper weaning trial. None of us perform at our peak when we are groggy.
3. Volatile Anesthetic agents are very cheap to use compared with other IV medications used for sedation (I know somewhere someone will be asking whether this is a cost-effective option – so the answer is yes).
4. You can wake your patient with very few if any lingering sedation effects which could potentially decreased failed weaning attempts due to other IV medications.
5. There is evidence that volatile anesthetic agents have protective qualities for organs. From what I understand (sorry I still have more reading to do) there is good evidence to support the idea that their cardiovascular protective qualities to Volatile Anesthetic Gases (SevoFlurane and IsoFlurane). I am also told that some believe there are protective qualities for other organs such as the liver, cerebrum, and kidney (not sure about the level of evidence here). Should also state that while these organ protective qualities are my understanding; I do not pretend to have done any great deal of research or reading on these yet, so you are required to do your own due diligence here. I will try and post more on this in the near future.
The really cool idea here is that most patients I have had on the ventilator have had some other multi-organ issues going on (i.e. cardiac, liver failure, kidney failure, etc). If this can provide some protection for other organs then that is just icing on the cake. I mean who doesn’t want something that will help improve outcomes.
Downsides to the AnaConDa
Yes everything has its limitations.
1) At present the AnaConDa adds a significant amount of dead space (about 100ml) so it is not considered appropriate if tidal volume can not be maintained at 350 mL or greater. Take away here is that it is not for small pediatric patients.
2) Active humidification is a contraindication. The AnaConDa functions as an HME and should not require active humidification.
3) There may be an initial capital equipment purchase required for a gas analyzer and/or scavenging system.
4) The AnaConDa like all other HME’s must be changed if patient secretions cause high resistance or every 24 hours (which-ever comes first).
5) The AnaConDa is not intended to be used in patients with copious secretions.
6) The AnaConDa is not intended to be used with Desflurane.
DECLARATION:
In case it is not already obvious the AnaConDa is a device I sell. While I think it has potential to add to the arsenal we have to deal with ventilated patients by improving outcomes in a cost-effective manner; I do stand to gain financially by the sale of these items.
Additionally the information above is correct to the best of my knowledge, but does not supersede instructions supplied by the manufacturer or does it necessarily cover all the potential issues that may occur with use. It is merely my take on what I believe to be a product with a lot of potential benefits for ventilated patients, staff and even budget.
UPDATED DECLARATION:
I can now say this is no longer and item that I sell as part of my portfolio. Having said that I still think it is a product with a lot of potential. To those who are using it, all my best. Please feel free to share your thoughts and experiences.






You must be logged in to post a comment.